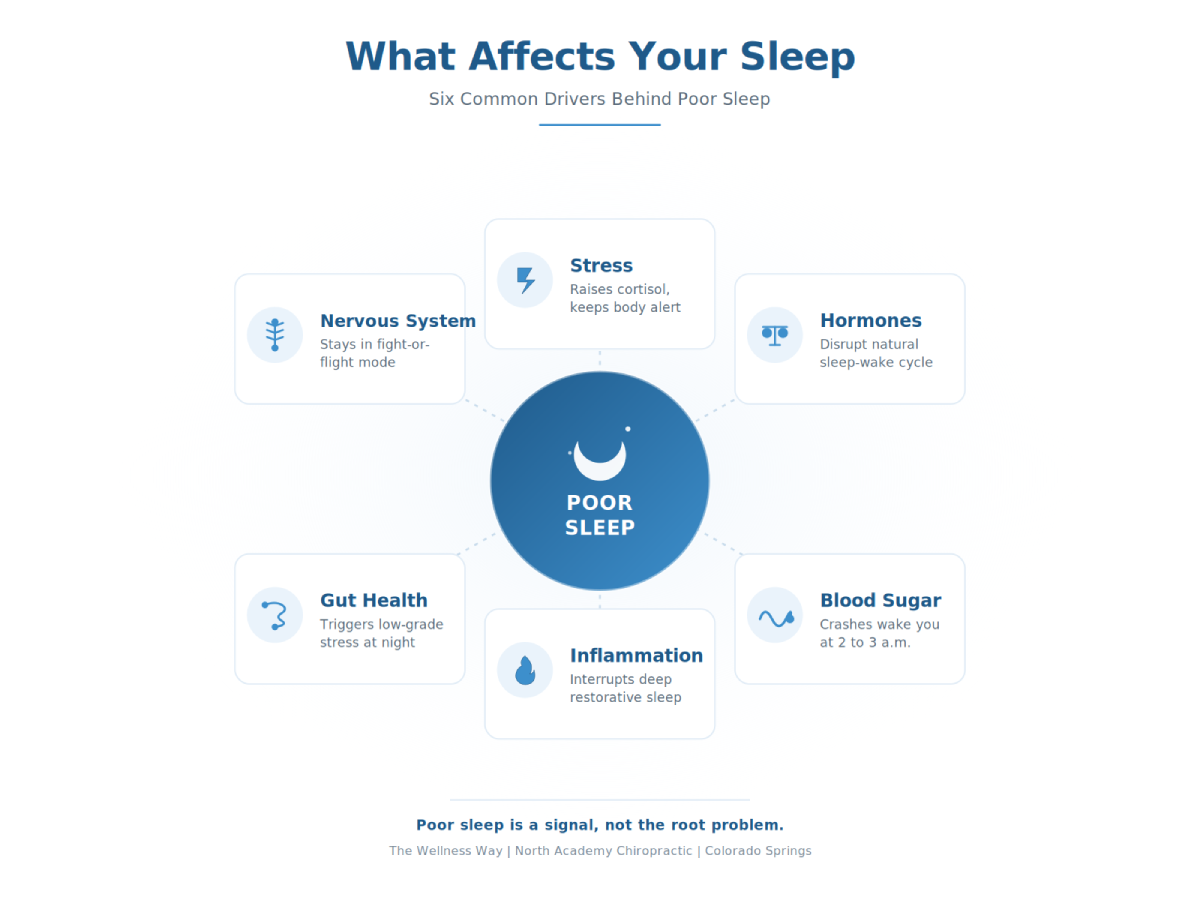
If you keep lying awake at night, waking up at 2 a.m. with your mind racing, or finally falling asleep only to feel like you never rested, you are not alone. The causes of poor sleep are rarely about willpower or going to bed earlier. At The Wellness Way, trouble falling asleep, waking through the night, sleeping lightly, or waking up unrefreshed are often signs that the body is under stress and struggling to adapt. Poor sleep is not usually the root problem. It is a warning light on the dashboard, and the goal is to figure out what it is pointing to.
Understanding Insomnia as a Sleep Disorder
Insomnia is one of the most common sleep disorders. It describes a persistent struggle to fall asleep, stay asleep, or feel rested in the morning, even when you have the time set aside for sleep. While the occasional bad night is normal, insomnia becomes a concern when it happens regularly and starts affecting how you feel during the day.
Acute vs Chronic Insomnia
Acute insomnia is short-term and usually tied to a specific stressor, like a deadline, a life change, or travel. It often resolves on its own. Chronic insomnia is when poor sleep happens at least three nights a week for three months or longer. Chronic patterns usually point to underlying imbalances that need attention, not just better sleep habits.
Sleep Is Not Just Rest
Sleep is recovery. Sleep is a hormonal balance. Sleep is a brain function. Sleep is immune support. Sleep is for repair. It is one of the main times your body does its deepest work, and when that process keeps getting interrupted, the body starts falling behind.
Signs and Symptoms of Insomnia
The symptoms of insomnia show up most clearly at night. You lie there, eyes open, mind running. Or you fall asleep quickly but wake an hour later and cannot drift off again. The patterns differ, but the underlying message is the same: the body is not getting the deep, restorative sleep it needs.
Common signs include:
- Trouble falling asleep, even when you feel tired
- Waking up several times during the night
- Waking up too early and being unable to fall back asleep
- Light, restless sleep that never feels deep
- Feeling unrefreshed in the morning, no matter how long you were in bed
- Anxious thoughts or a racing mind at bedtime
Poor sleep also tends to spill into the day. If you are dealing with ongoing daytime tiredness, brain fog, or low motivation, our page on fatigue and exhaustion goes deeper into what may be draining your energy.
Tired but Wired? That Is a Clue
One of the most frustrating patterns people experience is feeling completely exhausted but still unable to relax. Their body feels worn out, but their mind will not shut off. They finally fall asleep, only to wake up at 2 or 3 in the morning staring at the ceiling. That is often a sign that the stress response is too active. When the body is stuck in fight-or-flight mode, it has a hard time shifting into repair mode.
Causes of Poor Sleep
Most sleep conversations focus on surface-level solutions. Take a sleep gummy. Try melatonin. Maybe use a stronger sleep aid if that does not work. At The Wellness Way, we ask a different question: why is the body struggling to sleep in the first place? The causes of poor sleep are usually layered, and several stressors often stack on top of each other to tip the body out of its natural rhythm.
Stress and Cortisol Disruption
Chronic stress keeps cortisol elevated when it should be winding down. This is one of the biggest reasons people feel tired but wired at night. Your body cannot drop into rest mode if it thinks it still needs to stay alert.
Hormone Imbalance
Hormones like cortisol, melatonin, progesterone, and thyroid hormones all influence sleep. Imbalances during perimenopause, menopause, or periods of high stress can cause night waking, light sleep, and early morning wake-ups.
Blood Sugar Instability
If your blood sugar drops in the middle of the night, your body releases stress hormones to bring it back up. That can wake you up around 2 or 3 a.m., often with a racing mind for no clear reason.
Inflammation Does Not Clock Out at Bedtime
If inflammation is high, sleep often suffers. People usually think of inflammation as pain or stiffness, but it can also show up as restless sleep, poor recovery, and that sense that the body just cannot fully settle.
Food Sensitivities and Gut Health
The gut and the nervous system are deeply connected. Food sensitivities, blood sugar swings, and gut imbalances can all create a low-grade stress response that keeps the body from relaxing at night.
The table below breaks down the most common causes of poor sleep and what they often feel like in real life.
| Cause | How It Affects Sleep | What It Feels Like |
|---|---|---|
| Stress | Raises cortisol and keeps the body alert at night | Tired but wired, racing thoughts at bedtime |
| Hormone Imbalance | Disrupts the natural sleep-wake cycle | Frequent night waking, light or restless sleep |
| Blood Sugar Instability | Causes overnight crashes that signal the body to wake up | Waking around 2 to 3 a.m., sometimes with hunger |
| Inflammation | Interrupts deep sleep and slows recovery overnight | Restless sleep, stiffness, waking up unrefreshed |
| Food Sensitivities and Gut Issues | Trigger a low-grade stress response while you sleep | Bloating at night, poor sleep after certain meals |
| Nervous System Stress | Keeps the body in fight-or-flight mode | Cannot relax, mind will not switch off |
Risk Factors for Insomnia
Some people are more likely than others to develop ongoing sleep issues. Common risk factors for insomnia include:
- Age: Sleep patterns naturally shift with age, especially after 50.
- Chronic Stress: Long-term stress changes how the body regulates rest and recovery.
- Hormonal Changes: Pregnancy, perimenopause, menopause, and thyroid imbalances all affect sleep.
- Lifestyle Habits: Irregular schedules, late caffeine, alcohol, and screen use before bed all play a role.
- Underlying Health Conditions: Pain, digestive issues, and nervous system stress can interrupt sleep night after night.
- Mental Health: Anxiety and depression often disrupt sleep cycles, and the relationship runs both ways.
How Insomnia Is Diagnosed
There is no single test for insomnia. It is usually identified through a careful look at your sleep history, daily habits, and overall health. A sleep diary tracking when you go to bed, how often you wake up, and how you feel in the morning is often the first step. Some people may also benefit from lab work to check hormones, blood sugar, inflammation markers, or thyroid function. If poor sleep is paired with loud snoring, gasping, or extreme daytime sleepiness, a formal sleep study may be needed to rule out conditions like sleep apnea.
Treatment for Insomnia
There are several proven ways to help treat insomnia, and the best results usually come from combining a few approaches rather than relying on just one.
Cognitive Behavioral Therapy for Insomnia
Cognitive behavioral therapy for insomnia, often called CBT-I, is one of the most effective long-term treatments. It helps you change the thought patterns and habits that keep poor sleep going, including unhelpful beliefs about sleep, irregular bedtime routines, and the anxiety that often builds up around going to bed.
Addressing Root Causes Instead of Suppressing Symptoms
Sleep medications and over-the-counter aids may help in the short term, but they do not address why the body is struggling to sleep. The Wellness Way focuses on identifying what is driving poor sleep and supporting the body so it can recover its natural rhythm. That often means looking at stress, hormones, inflammation, gut health, and nervous system function together, not in isolation.
How to Sleep Better
If you want to know how to sleep better, the answer usually starts long before bedtime. Better sleep is built during the day. The way you eat, the way you respond to stress, the inflammation in your body, your hormone patterns, and your daily habits all shape what happens when your head hits the pillow.
Supporting the Nervous System Through Chiropractic Care
Chiropractic care supports the nervous system, the master communication system of the body. When the spine is not moving the way it should, and the body is carrying tension, it can be harder for the system to shift into a calm, restorative state. That is why one of the most common things we hear after an adjustment is, “I slept so well.” Patients come in for neck pain, headaches, or stress, and then come back saying the biggest surprise was how deeply they slept that night. Chiropractic does not treat sleep the way a sleep medication tries to knock someone out. It supports the body so it can do what it is designed to do better.
Daily Habits That Support Better Sleep
Try to:
- Get morning sunlight within an hour of waking
- Eat balanced meals with enough protein and fiber to steady blood sugar
- Limit caffeine after midday
- Cut back on alcohol, especially close to bedtime
- Keep a consistent wake time, even on weekends
- Build a short wind-down routine, slow breathing, lower the lights, and fewer screens
Sleep Is Not a Luxury, It Is a Signal
If your sleep is off, your body may be telling you something important. Maybe it is overwhelmed. Maybe it is inflamed. Maybe it is out of balance. Maybe it is asking for help, not just sedation. When people start sleeping better after chiropractic care and a more root-cause approach, it is often because the body is finally getting what it needs to heal.
Get Sleep Support in Colorado With The Wellness Way
If you are not sleeping well, do not ignore it. Listen to it. It may be one of the most important messages your body is sending. The causes of poor sleep can be identified, addressed, and improved with the right support.At The Wellness Way in Colorado Springs, we look at the full picture, stress, hormones, inflammation, gut health, and nervous system function, so you can finally sleep deeply and wake up feeling restored. Schedule a consultation, and let’s get to the root of what is keeping you up at night.